|
About Lymphoma > Symptoms & Complications of Lymphoma
Last update: 09/01/2014
|
TOPICS
General Symptoms | Alphabetical | B-symptoms | Other symptoms - neuropathy | Reporting Symptoms | Disease Direction Indicators | Blood counts | Ascites | Cutaneous (skin) | Itching (Pruritus) | Fatigue | Lymphedema | Nosebleed | Night Sweats | Pain | Pleural effusions | Performance Standards | Restless Leg |
Weight Loss (cachexia)
|
General symptoms
NOTE: This topic is for patients who already have a diagnosis of lymphoma.
Lymphoma is often first suspected when there are painless enlarged lymph nodes that persist and present in different parts of the body. Most of the time, enlarged lymph nodes are caused by infections and do not mean lymphoma. Only a biopsy and subsequent pathology evaluations of the tissue can determine or exclude the diagnosis of lymphoma. See also Before Diagnosis

Understanding the symptoms of lymphoma lets you better participate in your care and treatment.
Patients often report that it's difficult to distinguish between important symptoms and those that may be unrelated to lymphoma.

Some Related Definitions:
Blood tests can identify the underlying cause of symptoms that are common for lymphoma such as fatigue or bleeding, but not that it is caused by the lymphoma.
Anemia absolute reduction in the quantity of the oxygen-carrying pigment hemoglobin (Hgb) in the circulating blood.
Leukopenia low white blood cell count (WBC) less than 5.0 X 109/L
Lymphadenopathy abnormal increase in size of lymph nodes.
Thrombocytopaenia platelet count of less than 150 X 109/L)
|
General symptoms and signs of lymphoma
Alphabetical List | B-Symptoms | Systemic Symptoms | Reporting Symptoms
A Systems Checklist | Printable Symptoms Checklist (PDF)
"Because symptoms are what YOU experience,
your healthcare providers can only know about your symptoms if YOU tell them.
This puts you in the unique position of being the symptoms expert."
Charles S. Cleeland, PhD, with Diana Lazzell
The symptoms or signs of lymphoma will vary depending on the type of lymphoma, how advanced it, and where the lymphoma is actively growing. New symptoms will be worrisome of course ... and can be difficult to distinguish from unrelated causes, such as a new active infection.
It's important to notify our doctor about new and unexplained symptoms - especially if they persist or get worse over time. For this reason we have developed a checklist on how to report symptoms to our medical doctors.
The type of lymphoma will influence the types of symptoms that are most common. For example, gastric MALT lymphomas may present as an upset stomach; or a change in bowel movement could be caused by an enlarged lesion in the GI tract.
Systemic symptoms (or b-symptoms) such as unexplained fever and chills are most likely to appear in advanced stages of lymphoma or when there is steady progression.
Symptoms that negative impact our quality of life is an acceptable reason to start treatment for indolent lymphoma according to GELF and NCCN guidelines for Need to Treat
Lymphoma can directly or indirectly affect our performance as it advances. Taking part in regular exercise has direct benefits - can improve our general health, fitness and help to relieve anxiety. It is also a good way to monitor our performance, which might otherwise decline without notice. In this way we can report a decrease in our ability to do regular activities and more effectively inform your doctor, such as:
"I could walk around the block last week, but could only make it half the way today." Our doctors can interpret such reports with more confidence as we've provided a baseline that helps to gauge the significance of the change, which can guide how we are monitored. In contrast, it does not help as much if we can only report: "I feel more tired."
Symptom of Lymphoma or Unrelated?
Following a diagnosis of a lymphoma the mind often races -- we are prone to interpret each sensation as a sign of progression or relapse. Anxiety and fear can cause or contribute to our fatigue. Please discuss such fears with your doctors who can guide you through this and provide remedies of the appropriate kind if they are needed. See also Living Well with Lymphoma
Ask your doctor for guidance on the types of symptoms that should be reported immediately and how long to monitor other symptoms to see if they may be self limiting.
Lymphoma does not commonly present as a medical emergency. Symptoms that do not get worse or become less intense over time are often not related to lymphoma. However, if you have doubts and concerns, please report your symptom by phone to your medical team.
See Reporting Symptoms below.
Reporting symptoms:
"Most doctors and nurses report that one of the greatest barriers to good symptom management is a person’s unwillingness to report his or her symptoms. This silence often contributes to inadequate symptom management. Your input is a must if you are to receive the proper care for your symptoms."
Talking to Your Doctor about Symptoms http://bit.ly/dgctDj
Your honest and timely reporting of symptoms can be as important as any test.
Be sure to record and describe pain, fatigue, bowel and kidney function, fevers, sweats ... any change that is unexplained and persistent.
Patient reported symptoms (PRS) are an important part of managing lymphomas, but our accounts are admittedly subjective - can be magnified or downplayed, depending upon our temperaments ... can be related or unrelated to lymphoma ... so this is a problem and a common one at that.
NOTE: Sometimes our performance changes gradually and is difficult to notice. Therefore, a regular exercise program can be a good way to both improve your general health and monitor for changes, which will be more apparent when you have a regular exercise or activity program. As always, get approval from your doctor before starting an exercise program that might exceed your ability.
It can be difficult at times to identify the meaning of a symptom. Some symptoms may be common to certain stages of lymphoma and to specific treatments. Others may be explained by unrelated medical conditions, such as flu, an ulcer, a drug you are taking, or an injury you did not notice before.
When informing your doctor about a symptom also describe:
-
The intensity using a scale of 1 to 10
-
For visible symptoms, describe the size and appearance
-
When it started
-
How long it has lasted
-
If it waxes and wanes
-
The medications and supplements you may be taking and when you started taking them
-
How the symptom might change when you change position
-
If the symptom is associated with meals or specific foods
-
The time of day the symptom might be most intense
-
If you are also very anxious or depressed
These and other like details can assist your doctor in identifying the possible cause or causes, or if further tests are warranted.
Related Topics by PAL:
Alphabetical list of common symptoms
or laboratory abnormalities (signs):
It's important to report new unexplained symptoms - particularly when they persist or get worse over time.
Unexplained and persistent:
.gif) |
Anemia
a laboratory finding of low red blood count associated with the symptom of fatigue
from treatment or lymphoma
See Anemia for many causes
|
.gif) |
Appetite loss
a symptom such as from fullness
|
.gif) |
Fatigue
a symptom such as from anemia, or from depression
|
.gif) |
Fever
a symptom such as from advanced lymphoma but common to other conditions such as infection
|
.gif) |
Flu-like feeling
symptoms of aches, fever, chills, such as from advanced and progressing lymphoma but is also common to other condition such as the flu.
|
.gif) |
Infections
associated with a laboratory finding of low white blood cells*
Can be a complication of treatment or secondary to bone marrow involvement that can inhibit blood cell production leading to a higher risk of developing infection
|
.gif) |
Metabolic
a laboratory finding of high calcium, such as caused by too much vitamin D.
|
.gif) |
Night sweats
a symptom of drenching (change of clothing) sweats at night.
|
.gif) |
Neuropathy
A symptom that is common to some kinds of treatment and uncommonly a symptom of lymphoma
See also: Paraneoplastic neuropathies. [Curr Opin Neurol. 2013] - PubMed - NCBI http://1.usa.gov/1eeCnaN
And Diagnosis and management of paraneoplastic neurologic disorders.
Rosenfeld MR, Dalmau J. http://1.usa.gov/1dVzkbg
|
.gif) |
Pain
a symptom of lymphoma ... depending on the anatomic location that is secondary to pressure to bone or organs, or obstruction of bodily functions
|
.gif) |
Paraneoplastic syndrome:
An uncommon advanced symptom that may occur when there is very little detected levels of lymphoma.
These disorders arise from tumor secretion of hormones, peptides, or cytokines or from immune cross-reactivity between malignant and normal tissues. Paraneoplastic syndromes may affect diverse organ systems, most notably the endocrine, neurologic, dermatologic, rheumatologic, and hematologic systems. Paraneoplastic Syndromes (Mayo Clinic 2010)
|
.gif) |
Skin - Itchy skin
A symptom of lymphoma and many other medical conditions that is also called purititis.
|
.gif) |
Skin - Jaundice
an uncommon symptom of lymphoma that may indicate damage to liver from the treatment of lymphoma - yellowish tinge (related to liver function)
|
.gif) |
Swollen and painless lymph nodes
a common way that lymphoma presents as abnormal lymphocytes accumulate in these glands.
Can also be caused by a normal immune reaction to an infection
|
.gif) |
Swollen spleen
a fairly common symptom of lymphoma that can also cause a decrease in blood cell counts, leading to anemia or thrombocytopenia.
|
.gif) |
Thrombocytopenia - low platelets (bleeding)*
a laboratory finding that can be from treatment or from lymphoma, such as secondary to bone marrow involvement that can inhibit blood cell production. See Thrombocytopenia for many causes
|
.gif) |
Weight loss
a symptom of advanced lymphoma when unexplained by a change in diet. Can also be caused by a sense of fullness that reduces the appetite and intake of food.
|
B-symptoms
Systemic symptoms that are associated with advanced lymphoma that is progressing
New and persistent b-symptoms that are unexplained by other conditions (or by treatment) should be reported to your doctor:
Other symptoms related to area of involvement:
.gif) |
Localized pain
may occur depending on the location of tumors.
|
.gif) |
"If lymphoma occurs in the stomach or intestines
they may have gastrointestinal bleeding, a feeling of fullness, or abdominal swelling.
|
.gif) |
Lymphoma arising in the central nervous system
This is uncommon. It can cause neurological symptoms such as partial paralysis, seizures, confusion, and memory loss.
|
.gif) |
Lymphoma in the chest
can cause coughing, shortness of breath, and chest discomfort." 1 (MSKCC)
|
.gif) |
Swelling of limbs
|
General symptoms or signs may include:
.gif) |
Flu-like symptoms such as aches and pains.
|
.gif) |
Frequent infections from depressed immunity.
|
Since the symptoms of lymphoma are common to both minor and serious medical conditions, the diagnosis of lymphoma (which requires a biopsy) is often delayed. So called systemic or constitutional symptoms, such as fever, night sweats, weight loss in excess of 10%, or asthenia, are infrequent at presentation of the disease but can be observed in later stages. Progression to an intermediate-grade or high-grade lymphoma should be considered when a patient develops systemic symptoms.
Monitoring blood for increasing levels of LDH and Human beta-2 microglublin is commonly used to monitor progression. See LDH | Human beta-2 microglublin
A systems-based checklist:
My appointments with my oncologist include the following review of systems which I answer Yes or No for each individual symptom and add comments if necessary:
Do you now, or have you had, any problems related to the following systems?
.gif) |
Constitutional
B Symptoms: Fever, Chills, Headache, Other
|
.gif) |
Eyes: Blurred Vision, Double Vision, Pain, Other
|
.gif) |
Allergic/Immunologic: Hay fever, Drug Allergies, Other
|
.gif) |
Neurological: Tremors, Dizzy Spells, Numbness/Tingling, Other
|
.gif) |
Endocrine: Excessive Thirst, Too Hot/Cold, Tired/Sluggish, Other
|
.gif) |
Gastrointestinal: Abdominal Pain, Nausea/Vomiting, Heartburn, Other
|
.gif) |
Cardiovascular: Chest Pain, Varicose Veins, High Blood Pressure, Other
|
.gif) |
Integumentary: Skin Rash, Boils, Persistent Itch, Other
(an organ system that protects the body from damage)
|
.gif) |
Musculoskeletal: Joint Pain, Neck Pain, Back Pain, Other
|
.gif) |
Ear/Nose/Throat/Mouth: Ear Infection, Sore Throat, Sinus Problems, Other
|
.gif) |
Genitourinary: Urine Retention, Painful Urination, Urinary Frequency, Other
|
.gif) |
Respiratory: Wheezing, Frequent Cough, Shortness of Breath, Other
|
.gif) |
Hematologic/Lymphatic: Swollen Glands, Blood Clotting Problems, Other
|
.gif) |
Psychological: Are you generally satisfied with your life?, Have you considered suicide?
__________________
Provided by Sylvia (WebMagic)
|
Peripheral neuropathy as symptom of lymphoma (uncommon)
Muscle Nerve. 2005 Mar;31(3):301-13.
Lymphoma and peripheral neuropathy: a clinical review.
Kelly JJ, Karcher DS.
Department of Neurology, The George Washington University Medical Center, 2150 Pennsylvania Avenue NW, Washington, DC 20037, USA.
Abstract
Lymphoma occasionally affects the peripheral nervous system. When it does, the diagnosis can be elusive since many patients present without known lymphoma. Most peripheral nerve complications are due to non-Hodgkin's lymphoma (NHL), which infiltrates nerves causing axonal damage. This disorder can affect nerve roots and cranial nerves, often associated with lymphomatous meningitis. NHL may also infiltrate peripheral nerves and cause plexopathy, mononeuropathy, or generalized neuropathy. These neuropathies may resemble an asymmetric mononeuropathy multiplex or a generalized disorder such as chronic inflammatory demyelinating polyradiculoneuropathy.
When NHL infiltrates diffusely, the term neurolymphomatosis is used. Hodgkin's lymphoma (HL), by contrast, rarely infiltrates nerves. More often, HL causes immunological disorders of the peripheral nervous system such as inflammatory plexopathy or Guillain-Barré syndrome. Other rare lymphomas such as intravascular lymphoma and Waldenstrom's macroglobulinemia can also affect peripheral nerves in specific ways. In addition, other malignant and nonmalignant lymphoproliferative disorders enter into the differential diagnosis of lymphomatous neuropathy. This review discusses the multiple peripheral nerve presentations of lymphoma from the clinician's point of view and provides a guide to the evaluation and diagnosis of these uncommon, challenging disorders.
PMID: 15543550 http://www.ncbi.nlm.nih.gov/pubmed/15543550
See also Neurological complications of lymphomas http://www.ncbi.nlm.nih.gov/pubmed/17151523
In the News
.gif) |
* NEJM, 2013:
Probability of Cancer in Pulmonary Nodules Detected on First Screening CT http://bit.ly/14FeuuB
|
.gif) |
Medscape: Mindfulness Training Can Improve Symptoms, Mood After HSCT
|
.gif) |
Coping: Talking to Your Doctor about Symptoms http://bit.ly/dgctDj
|
Resources:
General symptoms:
-
MSKCC
-
Oncology Channel
-
|
|
Disease Direction indications
|
Disease Direction Indication
|
Increasing or decreasing lab values may help to gauge progression or response to treatment. However, location of disease can affect interpretation of the indicators provided here. Therefore, it's important to consult with your doctor about questions you may have.
Increased levels: ALT (sSGPT), Alkaline Phosphatase, AST (sGOT), Beta2-microglobulin, BIlirubin, Total Calcium, Creatinine, LD (LDH), Lymphocytes, Monocytes, Sodium, BUN, Uric Acid
Decreased levels: Albumin, Cholesterol, Globulin Iron, Total MCH, MCHC, MCV, Protein
.gif) |
SOURCE: NHL disease-specific disease Lab pattern indications CellMate Wellness
|
|
|
Abnormal Blood Counts
|
Abnormal Blood Counts
Anemia
(low red blood cells)
|
Blood counts cannot be reliably used to diagnose disease or monitor it, but abnormal counts are sometimes associated with lymphomas, leukemias, disease progression, or the side effects of treatment.
.gif) |
Leukocytosis emedicine.com
"refers to an increase in the total number of white blood cells (WBCs) from any cause. From a practical point of view, leukocytosis traditionally is classified according to the component of white cells that is contributing to an increase in the total number of white cells. Thus, leukocytosis may be caused by an increase in (1) neutrophil count (ie, neutrophilia), (2) lymphocyte count (ie, lymphocytosis), (3) monocyte count (ie, monocytosis), (4) eosinophilic granulocyte count (ie, eosinophilia), (5) basophilic granulocyte count (ie, basophilia), or (6) immature cells (eg, blasts). A combination of any of the above may be involved."
|
.gif) |
Leukopenia Merck Manual
"is usually characterized by a reduced number of blood neutrophils, although a reduced number of lymphocytes, monocytes, eosinophils, or basophils may also contribute to the decreased total cell count. Neutropenia accompanied by monocytopenia and lymphocytopenia is often a more serious disorder than neutropenia alone."
|
|
|
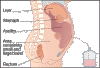
Ascites (not common)
|
Click to enlarge
|
 TOPIC SEARCH: PubMed and PubMed TOPIC SEARCH: PubMed and PubMed
Ascites is an excess of fluid in the membrane lining of the abdomen (the peritoneal cavity). Lymphoma might cause ascites by obstructing the lymphatic system. To relieve symptoms and diagnose the cause, a peritoneal fluid tap may be performed. Successful treatment of the lymphoma can resolve this problem.
"Ascites usually can be detected clinically by the presence of fullness in the flanks, shifting dullness, generalized abdominal distention with a fluid wave, and umbilicus eversion. In obese patients, moderate amounts of ascitic fluid may be difficult to detect. Ultrasound typically is performed to confirm the diagnosis in obese patients, because it can detect as little as 100 mL of fluid in the peritoneal cavity. Accumulation of fluid is first detected in Morison's pouch, then in the paracolic gutters; eventually, generalized ascites is noted."
postgradmed
Diagnosis "may be based on physical examination if there is a large amount of fluid, but imaging tests are more sensitive. Ultrasound and CT reveal much smaller volumes of fluid (100 to 200 mL) than does physical examination. Spontaneous bacterial peritonitis (SBP) (an infection of ascitic fluid) is suspected in a patient with ascites who also has abdominal pain, fever, or unexplained deterioration.
Diagnostic paracentesis (see Diagnostic and Therapeutic GI Procedures: Abdominal Paracentesis) should be performed if ascites is newly diagnosed, if its cause is unknown, or if SBP is suspected." The rare milky (chylous) ascites is most common with lymphoma. Merck manual
Treatment:
.gif) |
Case Report: Intraperitoneal rituximab: an effective measure to control recurrent abdominal ascites due to non-Hodgkin's lymphoma Springer-Verlag 2002
|
.gif) |
2012: Rituximab pharmacokinetics in ascites and serum in the treatment of follicular lymphoma with massive ascites http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3411293/
|
|
|
Cutaneous (skin)
|
|
|
Cutaneous lymphomas can present on anywhere on the skin.
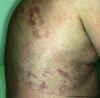
Image of Cutaneous B-Cell Lymphoma - Large Cell Type - Trunk
Click to enlarge
Source: Dermatologic Image Database
.gif) |
Lymphoma - Cutaneous B-Cell
|
.gif) |
Cutaneous B-Cell Lymphoma Large cell Type - Closeup of Right Scapular Area of Back
|
.gif) |
Cutaneous B-Cell Lymphoma - Large Cell Type - Right Scapular Area of Back - Detail of 2
|
Source: Aafp.org:
.gif) |
T-Cell Lymphoma Presenting as Benign Dermatoses - includes images aafp.org
|
|
|
Itching (Pruritus)
|
Itching (Pruritus)
|
 TOPIC SEARCH: PubMed TOPIC SEARCH: PubMed
Pruritus, also known as itch, is a common symptom of lymphoma.
.gif) |
Pruritus as a manifestation of systemic disorders.
Cutis. 1978 Jun;21(6):873-80. PMID: 657843 PubMed
|
.gif) |
Efficacy and safety of naltrexone, an oral opiate receptor antagonist, in the treatment of pruritus in internal and dermatological diseases. J Am Acad Dermatol. 1999 Oct;41(4):533-9. PMID: 10495371 PubMed
|
.gif) |
Severe pruritus should be a B-symptom in Hodgkin's disease.
Cancer. 1983 May 15;51(10):1934-6. PMID: 6831358 PubMed
|
.gif) |
Itch: scratching more than the surface. QJM. 2003 Jan;96(1):7-26. Review. PMID: 12509645 PubMed
|
|
|
Night Sweats
|
Drenching Night Sweats
|
Drenching night sweats is one of the so-called b-symptoms associated with lymphomas. This type usually " involves the entire body and are not confined to a specific hour during the night.
What causes night sweats in lymphoma? There does not appear to be a definitive answer. One possible mechanism behind night sweats is that the progression of lymphoma, and the body's way of fighting infection, have some things in common - both may require the mobilization of immune cells and cytokines (such as interferon, Interleukin); and that these immune activities might account for causing night sweats, fever, and achy muscles.
Your doctor will look at the possible meaning of night sweats in the context of other clinical symptoms and test results. It can be a sign of progression or transformation, depending on the severity and frequency. For this reason we believe it's prudent to notify your doctor when you have frequent night sweats to be sure.
You can assist your doctor in narrowing down the likely cause of the night sweats by providing key information :
.gif) |
How long have your night sweats occurred (days, weeks, months)?
|
.gif) |
Do they occur only at night
or do you experience drenching sweats at other times of the day?
|
.gif) |
Is your sleeping area too hot or crowded?
|
.gif) |
Have you had any recent illnesses?
|
.gif) |
Have you experienced any unexplained weight loss, fevers or shaking chills?
|
.gif) |
Are you taking any medications, large doses of vitamins, dietary or herbal supplements?
|
.gif) |
Do you have difficulty sleeping or been diagnosed with a sleep disorder?
|
.gif) |
Do you eat within several hours of bedtime?
|
.gif) |
Do you drink alcohol or use substances of abuse?
|
.gif) |
Have you recently traveled to other areas?
|
Possible triggers for night sweats include:
.gif) |
Environmental
uncomfortable room temperature, poor air circulation, too many blankets, thick sheets, close proximity to a bed partner
|
.gif) |
Emotional
stress, anxiety, disturbing dreams
|
.gif) |
Hormonal
hyperthyroidism, pregnancy, perimenopause or early menopause, hypoglycemic episodes in those with or without diabetes, others
|
.gif) |
Medications
certain antidepressants, niacin (high doses), tamoxifen, leuprolide, prednisone, drugs for erectile dysfunction (flushing and warm sensation), and high blood pressure. Even medications used to fight fever (aspirin, acetaminophen) can lead to rebound sweating as their effectiveness wears off.
|
.gif) |
Infections
such as tuberculosis, mononucleosis, human immunodeficiency virus
|
.gif) |
Medical conditions
such as gastroesophageal reflux disease, obstructive sleep apnea and chronic fatigue syndrome
|
.gif) |
Cancers Itching (Pruritus)
|
.gif) |
Neurological
concerns such as autonomic neuropathy or a delayed complication from a spinal cord injury."
|
Resources:
.gif) |
Diagnosing Night Sweats aafp.org | Stanford.edu
|
|
|
Nosebleed (not common)
|
Nosebleed
(not common)
|
 TOPIC SEARCH: PubMed TOPIC SEARCH: PubMed
Lymphoma can present in many ways, and the symptoms can have so many other causes. In a support forum I wrote in response to a question: " I've never heard of nose bleeds associated with lymphoma, but I suppose it's not out of the question." Then came two quick replies:
"My mother was also just diagnosed with NHL after recurring nosebleeds and a stuffy nose for about 6 months. There were no other symptoms." - Lesli (NHL-info)
"One of the symptoms which lead to my Mother's diagnosis of NHL was reoccurring nosebleeds." - Sandra (NHL-info)
|
|
Pleural effusions
|
Pleural effusions
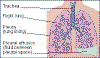
click to enlarge
|
 TOPIC SEARCH - PubMed TOPIC SEARCH - PubMed
Pleural effusions, or abnormal accumulations of fluid in the pleural space around the lungs, can be caused by a wide variety of diseases, including lymphoma. Sometimes an enlarged lymph node can block drainage of fluid that lubricates the pleural space. In such cases, successfully treating the lymphoma can resolve the condition. To relieve symptoms and diagnose the cause, a Thoracentesis, or pleural tap may be performed.
.gif) |
About Medline Plus * | Emedicine | Wikipedia.org
|
.gif) |
Thoracentesis or pleural tap (draining the fluid to relieve discomfort and diagnose cause) Medline Plus* | meddean.luc.edu
|
.gif) |
case report: Resolution of massive pleural effusion due to lymphoma with intrapleural interleukin-2. Elkadi D, Wiernik PH, Tong TR. http://www.ncbi.nlm.nih.gov/pubmed/20063279
|
|
Restless leg syndrome (not common)
|
Restless leg syndrome
(not common)
|
 TOPIC SEARCH: PubMed TOPIC SEARCH: PubMed
This syndrome can make it difficult to get adequate sleep because of pain or sensations experienced in the legs while sleeping. Restless leg syndrome might be related to an iron deficiency, which could be related to anemia.
.gif) |
About NIH
|
|
Weight loss - unexplained (Cachexia)
|
Weight loss - unexplained (Cachexia)
|
 TOPIC SEARCH: PubMed | Clinical Trials TOPIC SEARCH: PubMed | Clinical Trials
In the News
* Science Daily 2013:
Cancer Wasting Due in Part to Tumor Factors That Block Muscle Repair, Study Shows http://bit.ly/1cfGoRt
A symptom of lymphoma progression is weight loss that cannot be explained by diet. Cachexia, the loss of lean body mass, is most typically associated with advanced progression of the disease.
“The formal definition of cachexia is the loss of body mass that cannot be reversed nutritionally: even if the affected patient eats more calories” wikipedia.org
Is there a difference between weight loss and wasting?
"Yes. As its name implies, weight loss refers to a loss of body weight. Wasting syndrome refers to a loss of body mass or size, most notably muscle mass (sometimes referred to as "lean body mass"). Very often, both occur at the same time. However, this is not always the case. It is possible that someone who is losing weight might not lose muscle mass. It is also possible that someone losing muscle mass might not lose a lot of weight." beingalivela.org
You should report unexplained weight loss to your doctor or nurse and seek the underlying cause.
Some patients will try alternative diets that severely restrict calories. These diets can make it difficult to determine what is causing the weight loss, and they can be potentially dangerous if they contribute to wasting.
Related articles on weight loss, cachexia, and nutrition:
.gif) |
Cancer AND cachexia Related abstracts
|
.gif) |
Cancer Cachexia: Mechanisms and Clinical Implications PubMed
"It involves multiple pathways: ...signals from tumor cells, systemic inflammation in the host, and widespread metabolic changes (increased resting energy expenditure and alterations in metabolism of protein, fat, and carbohydrate). Whether it is primarily driven by the tumor or as a result of the host response to the tumors has yet to be fully understood."
|
.gif) |
Clinical Trials for Cachexia http://bit.ly/cmn53Y
|
|
|
|
![]() TOPIC SEARCH: PubMed
TOPIC SEARCH: PubMed![]() TOPIC SEARCH: PubMed
TOPIC SEARCH: PubMed
![]() TOPIC SEARCH - PubMed
TOPIC SEARCH - PubMed![]() TOPIC SEARCH: PubMed
TOPIC SEARCH: PubMed![]() TOPIC SEARCH: PubMed | Clinical Trials
TOPIC SEARCH: PubMed | Clinical Trials